This article is part of a series about why insurance carriers object to workers’ compensation reports and return them to the medical practice unpaid. This article is intended for medical providers, administrative staff, office managers, as well as insurance claims adjusters.
If you’ve been following our series on objections to workers’ comp reports, you know about the importance of including a complete history of symptoms, activities of daily living (ADLs), prior injuries, and examination in your visit note. If you’re covering these bases, then you should be getting payment for your workers’ comp visits!
Welcome to red flag #5 in our series, where we will discuss the importance of diagnostic tests.
Reason #5: Incomplete Diagnostic Tests
When you have a patient who has an unrateable injury, or a rateable injury that requires further diagnostic tests, the patient should be sent to a specialist so the injury can be examined further using diagnostic tests.
A diagnostic test is any test that aids in the presence or determines in the severity of pathology. Common diagnostic tests that are run on a patient due to a work injury include:
- X-ray
- Magnetic Resonance Imaging (MRI)
- Computed Tomography (CT) Scan
- Electromyography (EMG)
- Myelegram
In many cases, it may only be your responsibility to plug the results of the diagnostic tests into the impairment report. The results and measurements of the tests may be beyond your control, but that doesn’t affect your responsibility to make sure that they are accurately represented in your report.
To ensure that your report isn’t rejected by the insurance carrier, the results of the examination must be congruent with the results of the diagnostic test. This shows the insurance company that both you and the specialists running the diagnostic tests have done their work. If your examination concludes that your patient has a 70% range of motion in their arm, but the X-ray shows a shattered elbow, this means that someone isn’t doing their measurements correctly.
Authorizing Diagnostic Tests
When you order a diagnostic test, you must complete an RFA. Be sure to include the ICD-10 codes that demonstrate why the diagnostic test is necessary. There are online tools that can help you find the appropriate ICD-10 codes quickly.
Since it is the responsibility of the employers’ insurance to approve the RFA, an incomplete RFA form often delays treatment. The delay that can result from constantly denied RFAs alone can significantly impact the outcome of the payout for your impairment reports if your patient’s condition is improving or worsening in the meantime.
Make sure to take all of the necessary steps when filling one out. We have a blog post that tells you how to do just that.
If your medical practice uses RateFast as your workers’ comp solution, then RFAs are generated automatically as you order diagnostic tests (and other treatments).
Reporting the Results of Diagnostic Tests
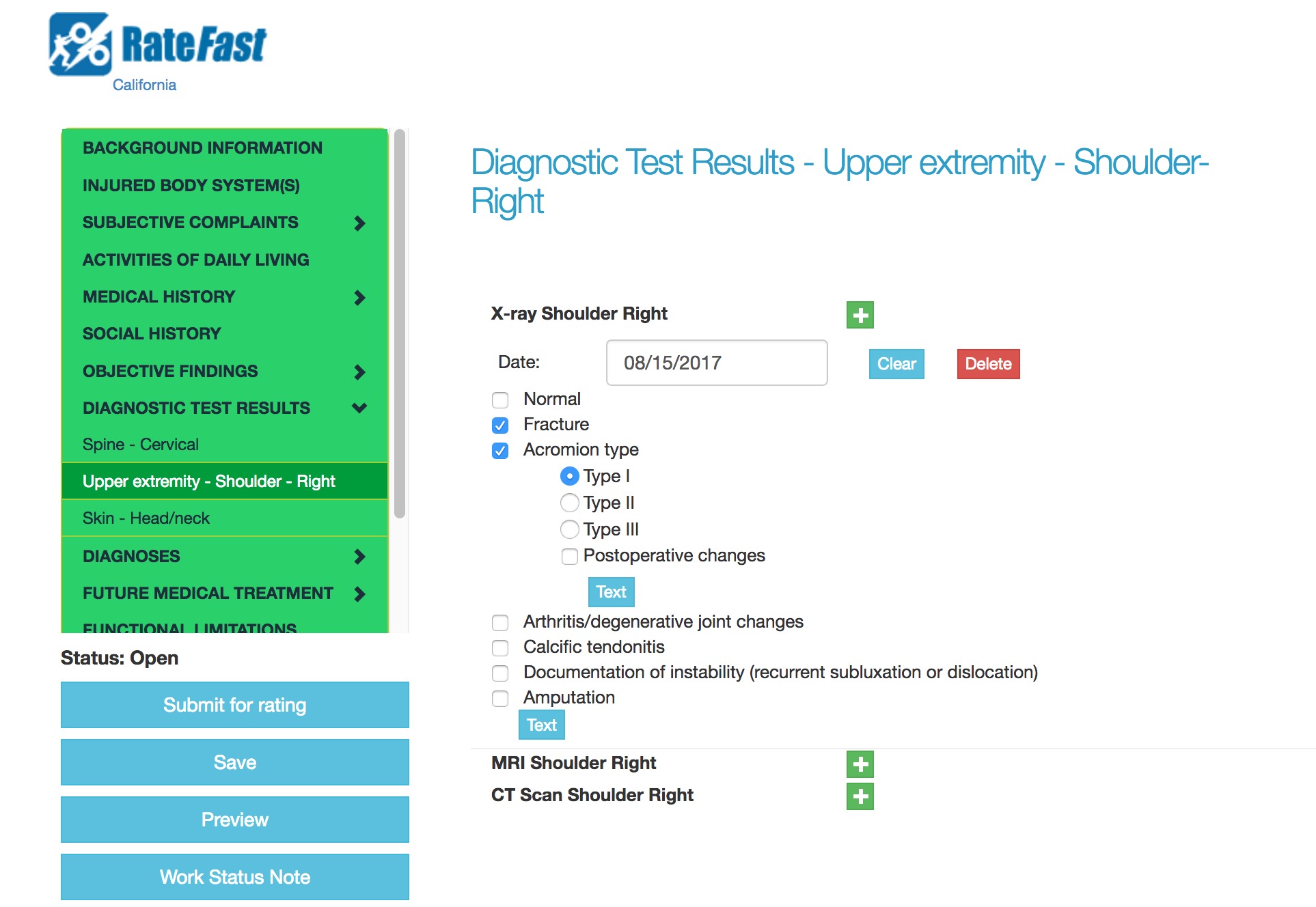
On a California Permanent & Stationary PR-4 report, you should include the results of all tests under the Diagnostic tests results (X-ray/Imaging/Laboratory/etc.) heading.
If you’re a RateFast user, you can enter the results of diagnostic tests in the “Diagnostic Test Results” section of a RateFast report. The results of a diagnostic test will be carried forward from report to report, and can be included or omitted in each report.
Conclusion
When another specialist is added to the equation, the risk for communication error goes up. This is true of almost every chain of communication. You can think of it like a game of “telephone,” where the risks of losing have much higher stakes.
That’s why it’s important to make sure all preliminary steps are handled, like filling out an RFA, including all ICD-10 codes. Once the test results are received, be sure to fill all the data out in your report. The specialist running the diagnostic test did all the work to ensure that their information was thorough, so do them the favor of passing that information along in your report.